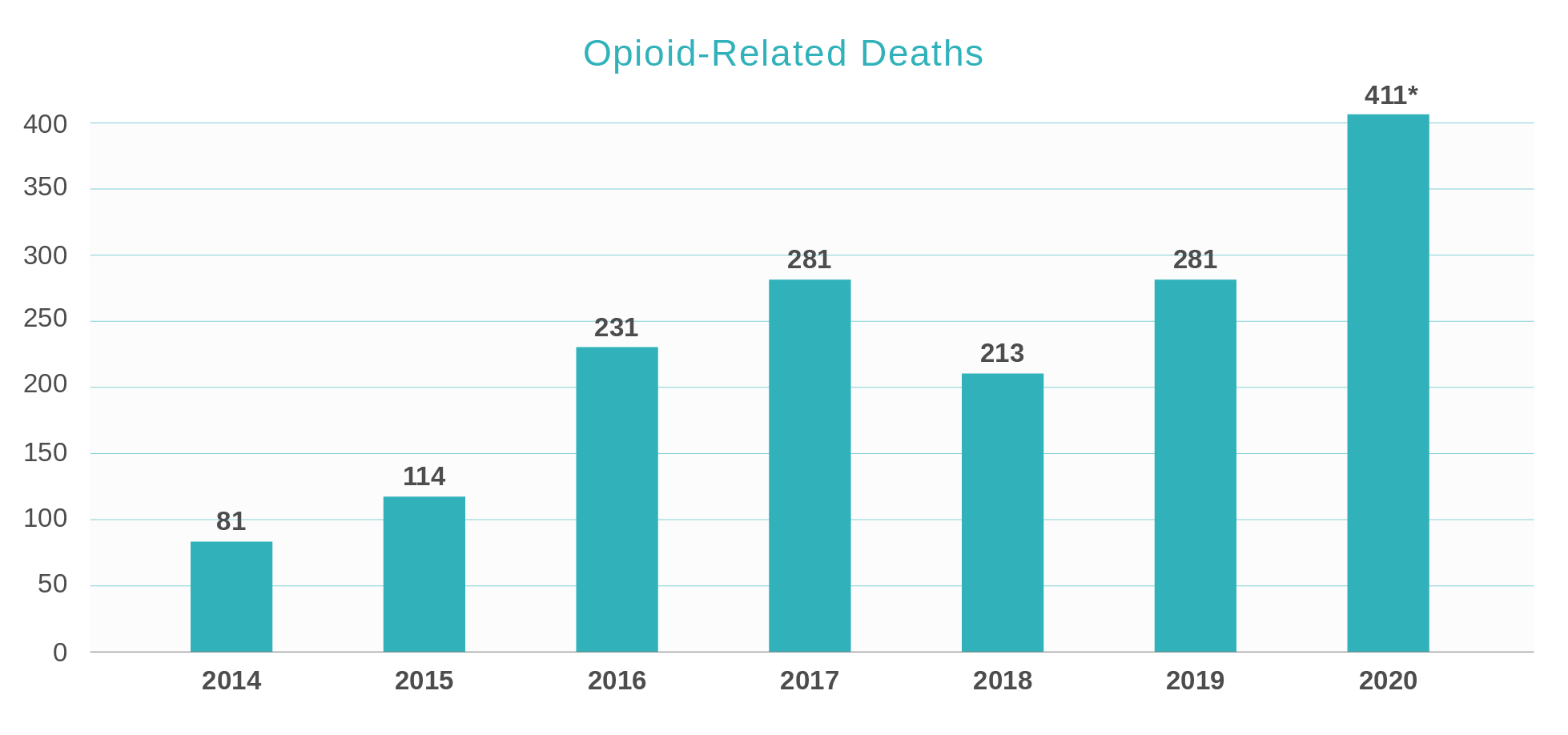
As opioid-related deaths continue to rise across the nation, Washington, DC has also experienced an alarming increase in fatal opioid overdoses. National trends largely reflect new opioid users who are White (non-Hispanic), younger adults who begin their addiction by experimenting with prescription drugs with the potential of progressing to heroin usage (Phillips, et.al, 2017). However, Washington, DC’s epidemic presents different trends in use. The graph below reflects the trend of fatal opioid overdoses since 2014. Fatal overdoses hit the first peak in 2017, with 279 overdoses, but declined in 2018 when we had begun implementation of an organized effort to combat the issue. In 2019, fatalities returned to the 2017 levels and hit an all-time high in 2020.
Washington, DC’s Epidemic in A Snapshot
- From 2016 to 2020, approximately 76% of all fatal opioid overdoses occurred among adults between the ages of 40–69 years old, and such deaths were most prevalent among people ages 50–59 (35%). During this time period, when there was a 50% increase in deaths overall, 50–59 year olds have seen a slight increase in deaths (6%), but other age groups have seen larger increases: 56% for 60–69 year olds; 129% for 20–29 year olds; 155% for 30–39 year olds; 1,200% for 70–79 year olds.
- Overall, 84% of all deaths were among African-Americans. This trend has remained consistent across years.
- Fatal overdoses due to opioid drug use were more common among males (72% of deaths were males in 2020).
- From 2016 to 2019, opioid-related fatal overdoses were most prevalent in Wards 5, 6, 7, and 8, with Ward 8 experiencing the most deaths.
- In 2020, 94% of fatal opioid overdoses involved fentanyl or a fentanyl analog (compared to 22% of cases in the first quarter of 2015).
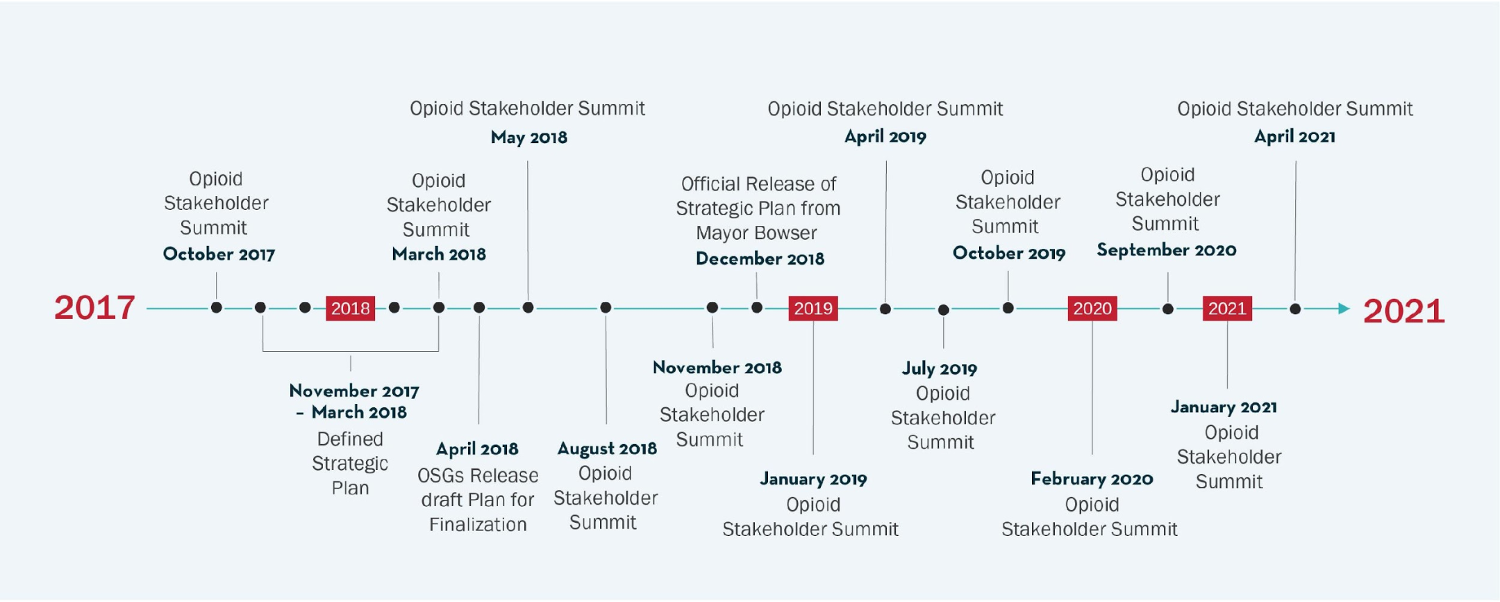
To comprehensively address the opioid epidemic in Washington, DC, local public and private partners must work together in a coordinated manner. This kind of partnership yields expertise in creating agile, cross-discipline, public-private leadership coalitions, rapidly aligning on targets and coordinated actions, and maintaining accountability on outcomes that will cause short- and long-term impacts. In October 2017, a group of 40 stakeholders, representing both the public and private sectors, convened for a Summit focused on how to jointly address Washington, DC’s opioid epidemic. Out of the Summit, the Strategic Planning Working Group was created.
In late November 2017, the working group members began to conduct stakeholder engagement sessions to assess the needs regarding prevention and early intervention, harm reduction, acute treatment, sustained recovery, and criminal justice. These sessions and the feedback from the working group members informed the draft plan, which was finalized at the end of February 2018.
In March 2018, the working group convened and membership for the seven Opioid Strategy Groups (OSGs) were formed to map out the implementation of the goals and associated strategies in the Plan. Leadership and membership of the OSGs were finalized in April 2018.
In 2020, an acknowledgement of the impacts of fentanyl on the rising death rate and the impacts of COVID-19 shifted the focus of the LLDC vision. The goal of LLDC has evolved to encompass a holistic, person-centered system of care that needs to be tackled at the community level. The OSGs reconvened in July 2020 to gather input and ideas from stakeholders on new LLDC strategies to inform the 2021 Plan revision (LLDC 2.0). The draft Plan was posted for public comment in March 2021.
Creating a person-centered system of care at the community level. Below is a group of stakeholders that has been working to achieve this vision.
Non-Governmental Agencies
- Amazing Gospel Souls Inc.
- AmeriHealth Caritas DC
- Aquila Recovery
- BridgePoint Healthcare
- Capital Clubhouse
- Children’s National Health System
- Community Connections
- Consumer Action Network
- DC Hospital Association (DCHA)
- DC Prevention Centers
- DC Primary Care Association (DCPCA)
- DC Recovery Community Alliance (DCRCA)
- Dreamers and Achievers Center
- Engage Strategies
- Family Medical and Counseling Services (FCMS)
- Fihankara Akoma Ntoaso (FAN)
- Foundation for Contemporary Mental Health (FCMH)
- Georgetown University
- George Washington University (GWU)
- Grubbs Pharmacy
- Hillcrest
- Honoring Individual Power & Strength (HIPS)
- Howard University
- Inner City Family Services
- IPRO QIN-QIO/Qlarant
- Johns Hopkins University
- MBI
- McClendon Center
- Medical Home Development Group (MHDG)
- Medical Society of the District of Columbia
- Miriam’s Kitchen
- Mosaic Group
- Oxford House
- Pathways to Housing
- Partners in Drug Abuse Rehabilitation Counseling (PIDARC)
- Pew Charitable Trusts
- Psychiatric Institute of Washington (PIW)
- Revise, Inc.
- Second Chance Care
- So Others Might Eat (SOME)
- Sibley Memorial Hospital
- Total Family Care Coalition
- United Medical Center (UMC)
- United Planning Organization (UPO)
- Unity Health Care
- Whitman-Walker Health
- Woodley House
- Zane Networks LLC
DC Government Agencies
- Criminal Justice Coordinating Council (CJCC)
- Council of the District of Columbia
- Department of Behavioral Health (DBH)
- Department of Corrections (DOC)
- Department of Forensic Sciences (DFS)
- Department of Health (DC Health)
- Department of Human Services (DHS)
- Department of Health Care Finance (DHCF)
- Department of Human Services (DHS)
- DC Public Schools (DCPS)
- Department of Aging and Community Living (DACL)
- DC Public Libraries (DCPL)
- DC Superior Court
- Executive Office of the Mayor (EOM)
- Fire and Emergency Services (FEMS)
- Homeland Security and Emergency Management Agency (HSEMA)
- Metropolitan Police Department (MPD)
- Office of the Attorney General (OAG)
- Office of the Chief Medical Examiner (OCME)
- Office of the Deputy Mayor of Health and Human Services (DMHHS)
- Office of the State Superintendent of Education (OSSE)
Federal Government Agencies
- Court Services and Offender Supervision Agency (CSOSA)
- Department of Justice (DOJ)
- Drug Enforcement Agency (DEA)
- Federal Bureau of Investigations (FBI)
- Federal Bureau of Prisons (FBOP)
- Pretrial Services Agency (PSA)



